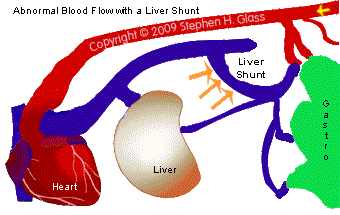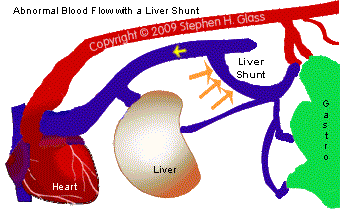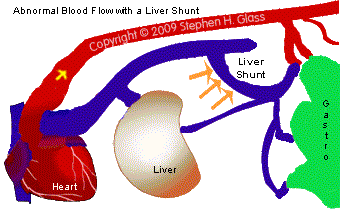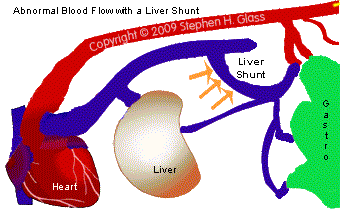
How is Liver Shunt Diagnosed?
This is frustrating since there is not just one test for this condition. One specialized test (Portogram) a veterinarian injects a contrast material (a liquid that looks white on x-rays) into the blood vessel in the abdomen. The injection can be performed through a surgical incision into the belly; by injecting the spleen directly through the skin; or by passing a catheter down the jugular vein (in the neck), through the heart, and towards the abdomen. Portograms usually require anesthetic and are invasive. The results show up on X-rays can outline the problem pretty clearly most of the time. But sinse this is an invasive test it makes it a poor choice for "screening" purposes. There are a number of possible abnormalities that might point towards a portosystemic shunt on routine labwork, including low BUN (blood urea nitrogen), low albumin, mild anemia, increases in ALT (serum alanine aminotransferase) or ALKP (serum alkaline phosphatase). If these hints are present, it would be a good idea to test the serum bile acid levels prior to eating and after eating. If this test is supportive of poor liver function then it may be a good idea to consider ultrasonagraphy and dye contrast X-rays.
How is it treated?
So far in my research I haven't found a cure for Liver shunt besides surgery for portosystemic shunts. As far as I know, dogs with extrahepatic shunts (occuring outside the liver itself) is easier to do than surgery in dogs with intrahepatic (inside the liver) shunts. If you know of a different cure please let me know.
CLINICAL DIAGNOSIS OF HEPATIC PORTO-SYSTEMIC SHUNTS by Larry Snyder, DVM
Clinical Signs: Most dogs will be diagnosed with port-systemic shunts under one year of age, but dogs as old as eight have been diagnosed with the condition. Animals are usually stunted, thin, depressed, have trouble gaining weight, and are usually characterized by the owners as chronic "poor doers". In most affected dogs there will be some degree of behavioral signs ranging from listlessness, apathy, or depression to more severe signs of circling, head pressing, stupor, drooling, blindness, or convulsions, some leading to coma. These behavioral changes are due to an accumulation of toxins (especially ammonia) that affect the brain causing a condition called Hepatic Encephalopathy. These toxins are most abundant in the blood stream following the dog eating, especially a high protein meal, & may remain high for hours afterward. Not all dogs with the shunt will show this meal associated behavioral change, but in 25% of the affected dogs that do, the diagnosis becomes clearer. A high percent of affected animals show an intolerance to anesthetics or tranquilizers, & will show increased recovery times following use of these products. Even anti-convulsants used to control seizures may be potentially dangerous if allowed to concentrate in a dog with functional shunt. Approximately 75% of affected individuals will show digestive system symptoms including poor appetite, ascites, vomiting, drooling, diarrhea, or occasionally deranged appetite (eating paper, etc.). Urinary system symptoms may include increased thirst and urination, & in a majority of porto-systemic shunt cases, there will be crystals or stones formed in the urinary tract. These crystals will be either uric acid or ammonium urate (ammonium biurate or thorn-apple crystals.). There can be bladder stones formed or crystals may be noted on the hair around the prepuce or vulva.
Laboratory Findings: Routine performed serum chemistries are fairly nonspecific toward confirming the diagnosis of porto-systemic shunts, but there may be a decreased total protein (primarily albumin), decreased blood glucose, decreased cholesterol, & decreased blood urea nitrogen (BUN). The uric acid levels may be elevated in a significant number of affected individuals. Acid levels are extremely important in the diagnostic screening of symptomatic potential shunts. Fasting and 2-hr. post meal blood samples are evaluated for bile acid levels. In virtually all porto-systemic shunts there will be a significant rise in the bile acid levels over normal. The use of bile acids in screening clinically normal dogs for liver shunts is not currently being advised due to the variation of normal bile acid levels in Yorkshire Terriers, & other breeds as well. Reports of recent vaccination with modified-live vaccines causing high serum bile acid levels in normal animals have not been confirmed as of this time. Liver function testing with Bromosulfaphthalein (*BSP.. Please read updated note below) or ammonia tolerance testing are sensitive & reliable if performed correctly. These tests measure the liver's ability to excrete/detoxify known agents, and thus measure liver function accurately.
Radiography. Radiography is one of the most important methods of establishing a diagnosis of porto-systemic shunt, & is currently the only universally accepted method of confirming a shunt, short of major surgery. Injection of a radiopaque dye into the spleen (Splenoportograpy) will show the shunt on radiographs & allow accurate assessment for surgical correction.
Nuclear Medicine. The placement of a radiopharmaceutical agent (radioisotope) specific for the liver into the colon for absorption through the mucosa has been gaining favor because of its noninvasive diagnostic value. This procedure requires expensive equipment & the diagnosis is based on the distribution of the radionuclide in the lung or heart compared to that in the liver. This procedure also does not identify the exact location of the shunt for surgical correction if required.
Ultrasound. Until recently, ultrasound was fairly unreliable for nonsurgical diagnosis of porto-systemic shunts. With the advent of Color Flow Ultrasound, there is the potential for diagnosis of this condition on non-anesthetized animals. At the present time, this technology appears to be the diagnostic procedure of choice. If currently undertaken research confirms its value, Color Doppler Ultrasound will soon be the preferred screening and diagnostic tool.
At the present time, Hepatic Porto-Systemic shunts are considered to be UNQUESTIONABLY genetic by some of the leading canine experts, but the mode has not been identified at the present time; research is being conducted at Michigan State University to identify this pattern. Genetic disorders in dogs can spread relatively rapidly if a dog, whether affected or a carrier, is a well-respected animal in either conformation or ability, and is used extensively for breeding. This is especially true in the case of the male that can produce hundreds of offspring during his breeding life. If the cause of such a condition can be discovered, then a working strategy can be implemented to control and eliminate the disorder.
The Yorkshire Terrier Club of America Foundation, Inc. is currently funding research into both the genetic nature of the problem & into the use of Color Flow Doppler Ultrasound as a diagnostic & screening tool. These steps will hopefully become the basis for setting up an open registry for Yorkshire Terriers & other affected breeds to hopefully eliminate, or at least minimize the problem within each breed.
What are the signs?
Most shunts cause recognizable clinical signs by the time a dog is a young adult but once in a while one is diagnosed at a later time in life. Since the severity of the condition can vary widely depending on how much blood flow is diverted past the liver it is possible for a lot of variation in clinical signs and time of onset of signs to occur. Often, this condition is recognized after a puppy fails to grow, making an early diagnosis pretty common, too. Signs of portosystemic shunts include poor weight gain, sensitivity to sedatives (especially diazepam), depression, head pressing (pushing the head against a solid object), seizures, weakness, salivation, vomiting, poor appetite, increased drinking and urinating, balance problems and frequent urinary tract disease or early onset of bladder stones. If the signs of problems increase dramatically after eating, this is a strong supportive sign of a portosystemic shunt.
4/10/2007 Dr. Tobias continues to work hard in her research to locate the gene
for liver shunt. She has been consulting with a genetic specialist.
While she has made significant progress, she is now at a point
where to be able to locate this gene, she needs be able to test 3
generations. She wouuld like to locate breeders who have 3 generations
in their line of liver shunt or MVD and would be willing to help. Dr. Tobias will
provide free dentals, spays/neuters for the breeders who participate.
Any interested breeder should contact Susan M. Schwarten - either by email (schwart@utk.edu) or at my office (865-974-5505) for additional information.